Sporotrichosis is an uncommon but a potentially staid fungal infection that can infect dogs, people or cats. The fact that this disease can be contracted by people from infected cats makes it serious and it should not be underestimated. Since this is not a common disease, owners or veterinarians may overlook Sporotrichosis as a possible reason of the symptoms.
What causes Sporotrichosis?
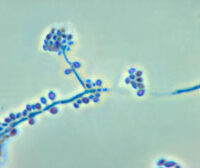
 Sporothrix schenkii is responsible for Sporotrichosis. This fungus has the potential to infect the respiratory system, the skin, the brain and sometimes the bones. The fungus infects through inoculation (inhalation or abrasions of the skin). It has an environmental origin; it is found naturally in the soil, sphagnum moss and plants. It can also be communicated zoologically in different animal species, and from animals to humans.
Sporothrix schenkii is responsible for Sporotrichosis. This fungus has the potential to infect the respiratory system, the skin, the brain and sometimes the bones. The fungus infects through inoculation (inhalation or abrasions of the skin). It has an environmental origin; it is found naturally in the soil, sphagnum moss and plants. It can also be communicated zoologically in different animal species, and from animals to humans.
Cats have a tendency to acquire a severe type of cutaneous sporotrichosis, this makes them have a higher chance of transmitting the disease to people and other animals. In-fact male cats that fight and roam outdoors are predisposed to puncture wounds which give S. Schenkii an advantageous route to get into the body. Sporothrix may also be communicated by other cats, often via scratches to the skin.
Other causes may include:
- Cat scratches which offer an increased chance of infection.
- Immunosuppressive infection should also be well thought-out as a risk factor.
- Clinically healthy cats using the same household with infected cats or exposure to infected animals is also risky.
- Animals around decaying organic debris in the soil tend to be predisposed.
Symptoms and Types
Cutaneous sporotrichosis
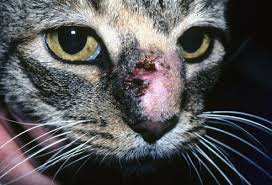
- Lesions, or bumps on the surface of the skin, swollen lymph glands
- Wounds which are associated with fighting may be found on the lumbar region, head or on the distal limbs
- Poor response to previous therapy in antibacterial
- Disease of the lymph (lymphadenopathy) is also common
- Previous puncture wound or trauma in the areas affected is a variable finding
- Combination of lymph and cutaneous form – normally an extension of the cutaneous type, which spreads through the lymph, leading to the formation of new draining tracts or crusts and nodules.
Disseminated sporotrichosis
- This is an uncommon form and is caused by an initial infection spreading into the body to a secondary area
- Systemic signs of fever and malaise
- When the infection spreads to the joints and the bones, it leads to oesteoarticular sporotrichosis
- When the infection spreads to the brain and the nervous system, it may cause sporotrichosis meningitis
- Symptoms include weight loss (cachexia) and loss of appetite (anorexia).
Pulmonary sporotrichosis
- Its occurrence is associated with inhalation of sporothrix schenkii spores
- There is more risk of developing pneumonia for infected animals.
Diagnosis of sporotrichosis in cats
This chronic disease has creeping progression and its symptoms are often subtle. It is hard to diagnose because many other infections have the same symptoms and thus must be ruled out. Patients for the disease will produce antibodies against the fungus, but because of the variability in specificity and sensitivity, it will not be a dependable diagnosis for the infection. The substantial diagnosis stands to be culturing the fungus from the cerebrospinal fluid, skin, synovial fluid and sputum.
Cats infected with sporotrichosis are exclusive in that the exudates from their lesions may be made up of numerous organisms. This leads to cytological evaluation of the exudates a expensive diagnostic tool in this species. Exudates with phagocytic and pyogranulomatous cells may contain yeast forms. Most of them are cigar-shaped but are also variable in size.
Treatment
Treatment of sporotrichosis in cats has given veterinary practitioners a great challenge. This is because the drugs that are mostly used have toxic adverse effects that are notable and they are also not permitted for use in animals.
Imidazoles
Sodium iodide has traditionally been used in diagnosis of sporotrichosis in cats; however, the agent has serious adverse effects leading to its replacement with safer and more effective antifungal drugs like imidazoles.
Itraconazole
Itraconazole has also been used in treating sporotrichosis in cats and is currently considered as the most efficient drugs in humans and also in cats. Due to its great selectivity for the fungal cytochrome system, Itraconazole is a potential inhibitor of a variety of fungal pathogens. Being a lipophilic drug, it is absorbed well after oral administration and widely spread to tissues such as the skin, where it gains a higher concentration than that in plasma.
In cats, it is administered orally at dosages of 5-10mg/kg (2.4-4.5 mg/lb) for every 12 hours. This should be preferably without food to increase rate of absorption. Compared to an equivalent dosage with the capsule formulation, the liquid type is considered because it allows for more accuracy in measurement of the dose. Again, it is efficiently absorbed if food is withheld and gains greater concentration than plasma.
Itraconazole has few associated side effects being reported in cats. During pregnancy, itraconazole administration is contradicted. Drug toxicoses have been reported in cats treated with antifungal agents. This will necessitate performance or regular serum bio-chemical analysis during sporotrichosis treatment. Treatment should be prolonged for one month after clear clinical cure to avoid clinical signs from recurring.
Ketoconazole
Ketoconazole has also been widely used but it has not led to comprehensive elimination of S.schenkii infection.
Prevention
As mentioned throughout this article, most of the cases of sporotrichosis are due to introduction of the fungus through a puncture or a cut in the skin while handling vegetation made up of fungal spores. As a cat owner, the disease can be prevented by wearing gloves and long sleeves while working with rose bushes, sphagnum moss, pine seedlings, hay bales and soil. This will minimize transmission when petting you cat.
Remember prevention also consists of immediate treatment of all wounds to you or your cat. Its also important to minimize cat fights, to reduce the risk of transmission.
Fortunately, sporotrichosis is very uncommon in dogs, people and cats. But we should always remember to check if our pets have non-healing sores or develop nodules, specifically if they are involve in cat skirmishes or spend more time in the woods.
If any symptoms of sporotrichosis are identified, it is important to report to a veterinary for immediate action. You should also see a physician for check-up; just in cases you are infected.
Thanks for The Cat Dandruff Clinic, if you found this article informative please like us using the side bar .


Comments are closed.